AMBROSE Cell Therapy – Kidney Disease Thesis
As is typical in a new research area, in 2010, a group of investigators did a mouse study to test the potential safety and effectiveness of adipose-derived stem and regenerative cells (ADRCs) to treat acute kidney disease.
The results were positive: The study demonstrated that ADRC-therapy drastically reduced mortality, with 100% of the treated mice surviving vs. 57% that got the placebo (controls), respectively. Likewise, the treated mice had significantly reduced serum creatinine levels (the key marker for kidney health) vs. the controls, respectively.[1]
Further investigations in small animals, large animals, and humans demonstrated that adult cell therapy prevented, and in some instances reversed, kidney disease progression. Two pilot studies using cultured adipose-derived stem cells (ADSCs) employing different delivery methods stand out:
- In 2018, a group from Chile published positive results with IV delivery of ADSCs to 6 renal failure patients,
- In 2019, Mayo Clinic issued a report detailing safety and strong signals of efficacy after injecting ADSCs in the spinal canals (intrathecal) of a not dissimilar group of patients.
In both cases, researchers reported reduced inflammation, lower serum creatinine levels, a reversal of fibrous scar (fibrosis), and improved blood flow. [2] [3] [4]
Spiral of Degeneration
Kidney failure follows a degenerative process similar to other chronic diseases. Trauma, environmental toxins, unhealthy lifestyle choices, hereditary factors, or a combination of these bad actors trigger an inflammatory response. Short-term inflammation (acute) is essential for repairing the body. This sort of inflammation is usually short-lived, disappearing once the healing process has taken place.
It is chronic systemic inflammation that becomes a problem.[5] Systemic inflammation, or inflammaging, is a common factor in a broad spectrum of severe, debilitating, and, sometimes, life-threatening conditions, including renal failure.[6] [7]
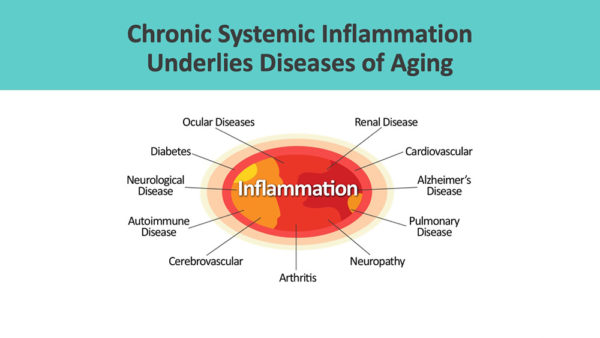 In the case of degenerative diseases, chronic inflammation begins a vicious degenerative process. That inflammation recruits the immune system, which exists to fight infections and to assist in healing. The immune system is our body’s military police force.
In the case of degenerative diseases, chronic inflammation begins a vicious degenerative process. That inflammation recruits the immune system, which exists to fight infections and to assist in healing. The immune system is our body’s military police force.
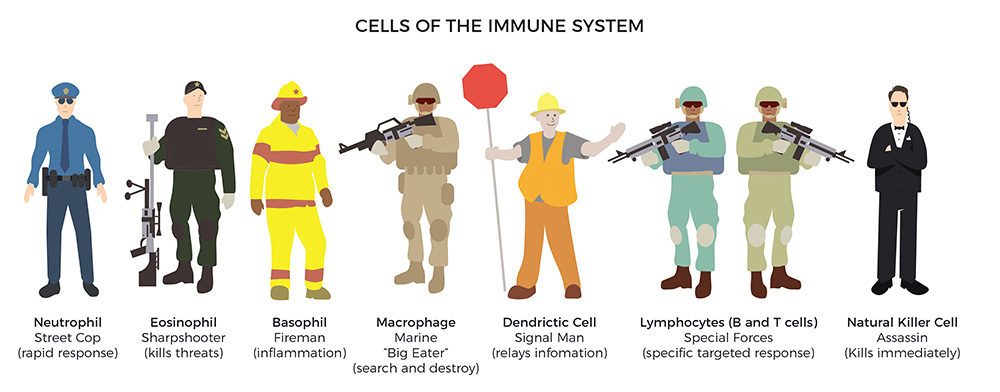
When immune cells sense the enemy, they send out troops of molecules called “cytokines” to fight them off. But the immune system can go out of control. An abnormal inflammatory-immune response is like having a backseat driver overreacting while “helping” you drive your car.
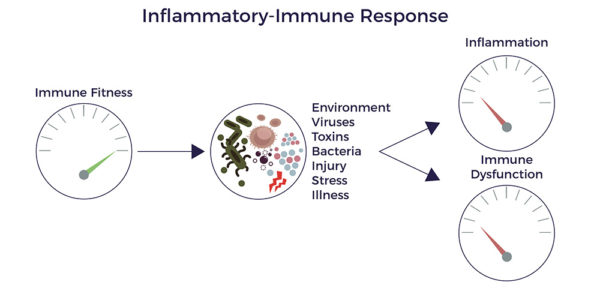
The immune dysregulation then leads to reduced blood flow (ischemia). Without adequate circulation, cells die off, scars and fibrosis form, tissues, and organs degenerate.
We call this the Spiral of Degeneration
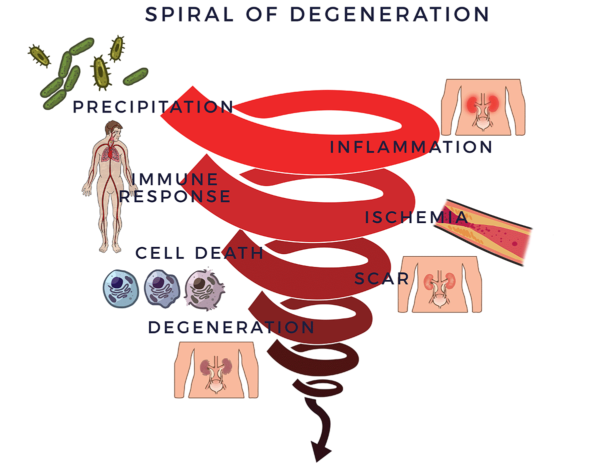
Loss of kidney function corresponds with inflammation affecting the kidney’s filtering system and their small blood vessels. The early stages are usually without symptoms. As kidney function worsens, the number and severity of symptoms rear their ugly heads. Eventually, patients are required to purify their blood with dialysis, a substitute for the kidney’s normal function.
Process of Repair
On the other side of the coin, ADRCs, through cell-to-cell communication, mobilize nearby cells to work more efficiently. This activity is called the paracrine effect.
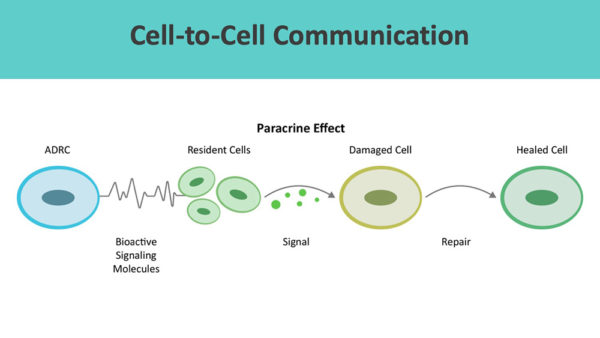
ADRCs are like a highly specialized fire department. When reintroduced into the bloodstream, tissues, or organs, the firefighters home to inflammation sites and release hundreds of bioactive signaling molecules. These cytokines recruit resident cells, who act as repair engineers, at the site of injury or disease. The local cells further release cytokines that decrease inflammation and modulate the overactive immune responses. They also release growth factors that stimulate new blood vessel growth. More blood supply reverses programmed cell death and reduces scar size. The regeneration of tissue and nerves follows. This process is how the body heals wounds – sometimes, it just needs reinforcements.
We call this the Process of Repair.

The factors in the Spiral are known to be involved with renal failure. The clinical trials for kidney disease show that the multiple repair mechanisms of the ADRCs can potentially reverse those factors. [8] [9] [10]
Summary
ADRCs have multiple attributes that are potentially helpful to kidney disease patients. Clinical-grade ADRCs can be prepared and delivered at the point of care.
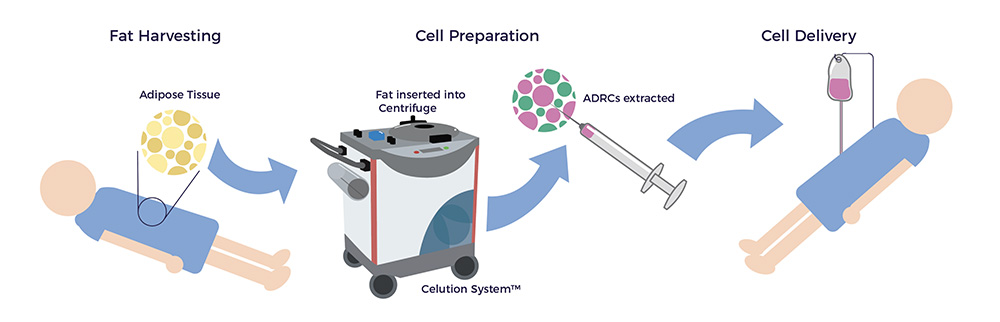
To learn about more ADRCs, please see Why Adipose Tissue.
To find out if you are a candidate for AMBROSE Cell Therapy, click here.
[2] A Eirin et al Adipose tissue-derived mesenchymal stem cells improve revascularization outcomes to restore renal function in swine atherosclerotic renal artery stenosis Stem Cells. 2012 May; 30(5): 1030–1041
[3] A Abumoawad In a Phase 1a escalating clinical trial, autologous mesenchymal stem cell infusion for renovascular disease increases blood flow and the glomerular filtration rate while reducing inflammatory biomarkers and blood pressure Kidney International (2020) 97, 793–804
[4] C Donizetti-Oliveira Adipose Tissue-Derived Stem Cell Treatment Prevents Renal Disease Progression Cell Transplantation, Vol. 21, pp. 1727–1741, 2012
[5] S. Amor Inflammation in neurodegenerative diseases Immunology, 129, 154–169
[6] C. Franceschi and J. Campisi Chronic Inflammation (Inflammaging) and Its Potential Contribution to Age-Associated Diseases J Gerontol A Biol Sci Med Sci 2014 June;69(S1): S4–S9
[7] Suliman ME, Stenvinkel P. Contribution of Inflammation to Vascular Disease in Chronic Kidney Disease Patients. Saudi J Kidney Dis Transpl 2008;19:329-45
[8] A Nguyen, A et al Stromal vascular fraction: A regenerative reality? Part 1: Current concepts and review of the literature Journal of Plastic, Reconstructive & Aesthetic Surgery (2016) 69, 170e179
[9] Guo et al Stromal vascular fraction: A regenerative reality? Part 2: Current concepts and review of the literature Journal of Plastic, Reconstructive & Aesthetic Surgery (2016) 69, 180e188
[10] JK Fraser PhD and S Kesten MD Autologous Adipose Derived Regenerative Cells: A platform for therapeutic applications Advanced Wound Healing Surgical Technology International XXIX
