Is a Golden Era of Spine Care Ahead?
In 2016, Barbara suffered from debilitating spinal stenosis. After failing to respond to chiropracty, physical therapy, medication, and steroids, Barb accessed a new option: The stem cells and other regenerative cells residing in her fat or adipose-derived regenerative cells (ADRCs). Five years since her treatment, Barb says that cell therapy “saved my future.”
In 2018, Trish, Jeff, and Kathy lived with complex, debilitating health conditions, including spine-related pain. After they had failed to get relief from conventional and integrative medicine, each chose to exercise their Right to Try AMBROSE Cell Therapy under the Federal Right to Try Act of 2017. Remarkably, over two years post-cell therapy, they all report their spine-related symptoms and dysfunction don’t hold them back anymore. But what is the scientific back story that led to their sustained outcomes? And what was the catalyst for a Golden Era of Spine Care?
Is Conventional Spine Care Antiquated?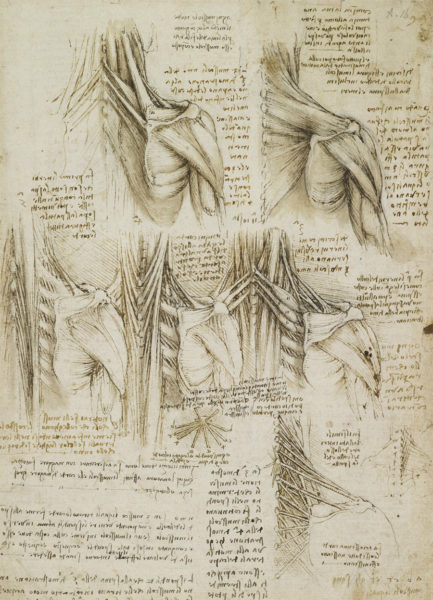 Spine care has its origins in antiquity. The Edwin Smith surgical papyrus, an Egyptian document written in the 17th century BC, is the first known discussion of neck and back-related injuries. Hippocrates (4th century BC) experimented with traction or local pressure to correct spinal deformities. Aristotle also contributed to our current day understanding of the neck and spine.
Spine care has its origins in antiquity. The Edwin Smith surgical papyrus, an Egyptian document written in the 17th century BC, is the first known discussion of neck and back-related injuries. Hippocrates (4th century BC) experimented with traction or local pressure to correct spinal deformities. Aristotle also contributed to our current day understanding of the neck and spine.
Few individuals in history have made as many contributions to so many disciplines as Leonardo da Vinci. Included in his vast body of work, Da Vinci sketched the first accurate depiction of the spine. [1]
As a result, knowledge of the neck and back, and their related disorders, have evolved since the Renaissance Man’s illustrations.
Early researchers proposed that neck and back pain resulted from the stress of heavy loads and age-related wear and tear on the discs. Then, in 1978, White and Panjabi published Clinical Biomechanics of the Spine. Here, they connected all the mechanical factors involved in neck and back health. Technically speaking, they found that in addition to vertebrae, our muscles, tendons, ligaments, blood vessels, and nerves (soft tissues) play significant roles in spine health and disease. White and Panjabi named those pieces of the puzzle the Functional Spine Unit (FSU).
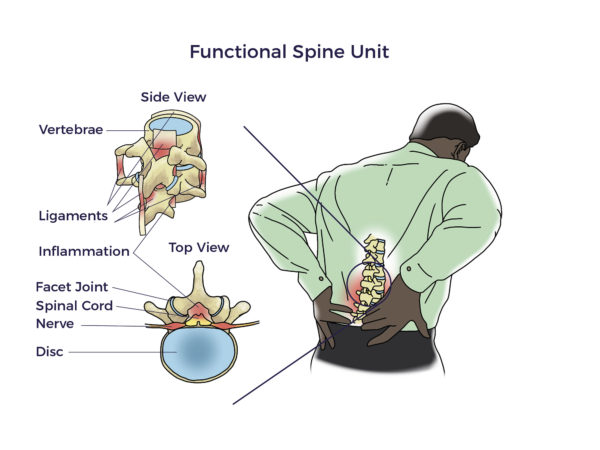 But there was still more to be discovered than the FSU. More recently, researchers began focusing on the vicious interplay involved with traumatic injuries, wear and tear, inflammation, and other diseases (co-morbidities). For example, patients with heart disease, diabetes, neurologic conditions, and autoimmune diseases have a higher prevalence of spine disorders than others without those conditions. In fact, Barb, Trish, Kathy, and Jeff each lived with other chronic debilitating conditions, including arthritis, hypermobility, kidney failure, and spinal cord injury, respectively. [2] [3] [4] [5]
But there was still more to be discovered than the FSU. More recently, researchers began focusing on the vicious interplay involved with traumatic injuries, wear and tear, inflammation, and other diseases (co-morbidities). For example, patients with heart disease, diabetes, neurologic conditions, and autoimmune diseases have a higher prevalence of spine disorders than others without those conditions. In fact, Barb, Trish, Kathy, and Jeff each lived with other chronic debilitating conditions, including arthritis, hypermobility, kidney failure, and spinal cord injury, respectively. [2] [3] [4] [5]
In 2001, Patricia Zuk, Ph.D. et al., working in a UCLA lab, accomplished a (non-obvious) leap forward for patients living with neck and back pain. Zuk’s group discovered mesenchymal stem cells (MSCs) were residing in adipose tissue. But how did their seemingly unrelated research catalyze a Golden Era of Spine care? We will answer that in a moment first; why was a new regenerative option needed in the first place?
Failed Back Surgery Syndrome
Despite those thousands of years of research and development, more people than ever are suffering from spine-related pain. Besides contributing to the opioid epidemic, the number of spine surgeries increases year in and year out.
Unfortunately, downsides to spine surgery, including high rates of complications, readmissions to the hospital, and poor outcomes, are common. [6] [7] As a result, approximately 4 million individuals live with failed back surgery syndrome (FBSS) in the U.S. Tragically, a spinal fusion gone wrong caused Jeff’s spinal cord injury.
Doctors call those with FBBS and others unwilling to risk a surgical intervention “no-option patients. Jeff’s spinal cord injury resulted from a spine surgery, which upon a second opinion, turned out to be unnecessary in the first place. Barb, Kathy, and Trish opted not to pursue surgery out of concern for those risks.”
Is there more to spine health than meets the eye?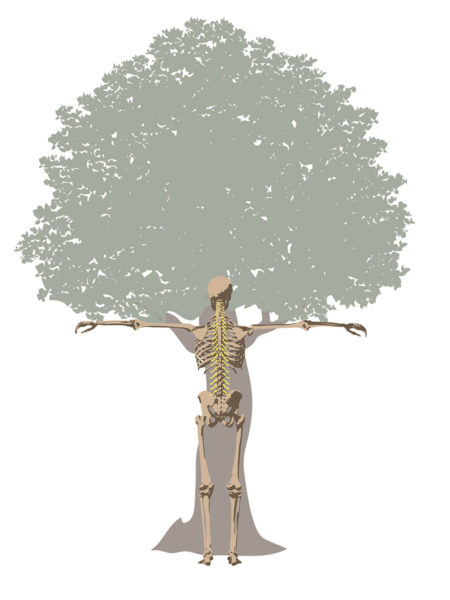 Circling back, in the early 1500s, Leonardo da Vinci took an unusual interest in tree anatomy. His Rule of Trees explained the balance between the trunk and branches of a tree. He counted the rings in tree trunks to determine “the nature of past seasons.”
Circling back, in the early 1500s, Leonardo da Vinci took an unusual interest in tree anatomy. His Rule of Trees explained the balance between the trunk and branches of a tree. He counted the rings in tree trunks to determine “the nature of past seasons.”
Perhaps it wasn’t coincidental that he sketched the spine, tree trunk, and branches, respectively? Let’s look at it this way: The tree’s trunk supports the crown and branches. Likewise, a healthy neck and back do the work of a strong tree. But even the strongest and thickest tree branch cannot handle a heavy load if the tree’s trunk is weak. Similarly, our legs, arms, hands, and feet can be affected by a degenerated FSU.
Ideally, our spines are a harmony of functional bones and soft tissues. The back and neck rely on all those elements to hold us upright and be mobile. But when the soft tissues atrophy or become arthritic, they pressure nerves, thus contributing to spine-related symptoms.
- Trish lived with sciatica, numbness, stiffness, and pain.
- Kathy’s bad neck kept her awake at night.
- Barbara’s situation prevented her from working, gardening, driving, and pottery.
Most vexing, back-related discomfort doesn’t discriminate: Gardners, crossfitters, weightlifters, golfers, and aging couch potatoes can end up unable to function without pain for varied reasons. [8]
ADRCs – the Spine’s Arborist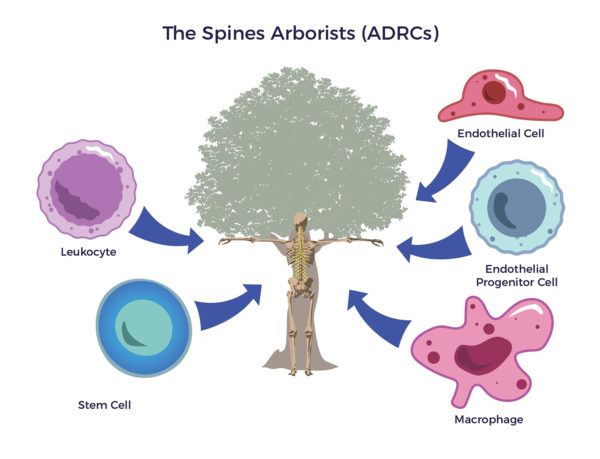 An arborist cultivates trees; tree removal is a last resort. The first thing that goes through their minds is how to save the tree. To do their jobs, arborists cultivate the whole tree. They use fertilizer, irrigation, and other regenerative tools to restore the tree’s trunk, limbs, and leaves.
An arborist cultivates trees; tree removal is a last resort. The first thing that goes through their minds is how to save the tree. To do their jobs, arborists cultivate the whole tree. They use fertilizer, irrigation, and other regenerative tools to restore the tree’s trunk, limbs, and leaves.
Around 2010, Zuk’s discovery of stem cells in fat came into play when some innovative doctors began treating spine patients with ADRC-based protocols. Their strategy was not dissimilar to an arborist’s. They recognized that a veritable pharmacopeia in a person’s fatty tissue could reduce arthritis and regenerate the supportive soft tissues in the neck and lower back. Back surgeries change the anatomy while cell therapy is, well, therapeutic.
Just as an arborist uses an array of skills to rehabilitate diseased trees, ADRCs use multiple mechanisms of action to rehab the FSU. At least as necessary, ADRCs restore balance or homeostasis in the systems that feed, care for, and defend the spine. In other words, better vascular, immune, metabolic, and nervous system wellness contributes to overall improvements.
In summary, not only did AMBROSE cell therapy help Barb, Jeff, Kathy, and Trish avoid risky surgeries, but all reported being more active, increased energy, and an improved sense of wellbeing.
[1] Bowen G et al Leonardo da Vinci (1452–1519) and his depictions of the human spine
Childs Nerv Syst (2017) 33:2067–2070
[2] M. Shamji et al. Proinflammatory Cytokine Expression Profile in Degenerated and Herniated Human Intervertebral Disc Tissues Arthritis Rheum. 2010 July; 62(7): 1974–1982
[3] J Gallo Inflammation and its resolution and the musculoskeletal system J Orthop Translat. 2017 July; 10: 52–67
[4] Asadian et al. Diabetes Mellitus, a new risk Factor for lumbar spinal stenosis: a Case–Control study. Clinical Medicine Insights: Endocrinology and Diabetes 2016:9 1–5
[5] Lotan R, Oron A, Anekstein Y, Shalmon E, Mirovsky Y. Lumbar stenosis and systemic diseases: is there any relevance? J. Spinal Disord. Tech. 2008;21(4):247-51.
[6] Camino Willhuber et al. Analysis of Postoperative Complications in Spinal Surgery, Hospital Length of Stay, and Unplanned Readmission: Application of Dindo-Clavien Classification to Spine Surgery Global Spine Journal July 2018
[7] Chase D. The opioid crisis is partly fueled by insurers and employers’ approach to back pain. StatNews. statnews.com/2019/03/27/opioid-crisis-insurersemployers- back-pain/. Published March 27, 2019.
[8] J Abbas et al Paraspinal muscles density: a marker for degenerative lumbar spinal stenosis? BMC Musculoskeletal Disorders (2016) 17:422
